A pioneering model has been unveiled that revolutionizes the evaluation of medical artificial intelligence (AI), moving beyond simplistic written exams based on historical data. This innovative approach tests AI in a virtual hospital that mirrors real clinical settings with unprecedented accuracy. By pre-emptively assessing the ripple effects of AI prescriptions on patient outcomes and resource allocation, researchers have established a crucial preclinical checkpoint to rigorously evaluate AI safety without risking actual patient lives.
On Tuesday, Dr. Kim Sung-eun from Seoul National University Hospital’s Specialized Research Institute, in collaboration with a Harvard Medical School team, introduced the Clinical Environment Simulator (CES). This groundbreaking tool dynamically evaluates medical AI powered by large language models (LLMs). The study detailing this digital virtual hospital assessment framework has been published in the latest online edition of Nature Medicine, a prestigious international journal with an impact factor of 50.
Traditional medical AI evaluations were limited by their reliance on static historical data, failing to capture the complex, cascading effects of real-time medical decisions. In actual clinical settings, patient conditions fluctuate rapidly, and each prescription directly impacts the hospital’s finite resources. Previous evaluation methods couldn’t account for these intricate temporal and systemic interdependencies.
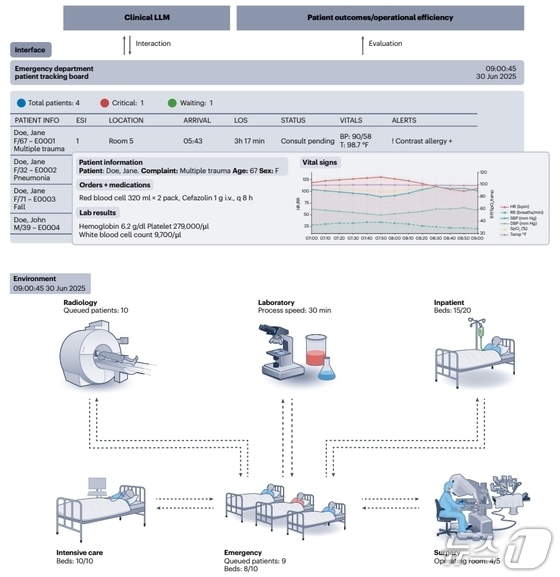
Recognizing this gap, the research team posited that medical AI should be tested for its adaptability within real-world time and resource constraints. To achieve this, they synchronized two core engines. The Patient Engine dynamically generates diverse virtual pathways of symptoms and treatment responses, drawing from disease trajectory templates defined by specialists and initial data from real electronic medical records. This engine effectively simulates the ever-changing nature of patient conditions.
Working in tandem, the Hospital Engine replicates the minute-by-minute workflow of actual hospitals. Using real-time data, it tracks bed availability, staff allocation, and equipment status with pinpoint accuracy. When a blood test is ordered, the system assigns the necessary medical personnel sequentially, mirroring real-world time frames. It even implements a sophisticated triage system, prioritizing resource allocation for critically ill patients.
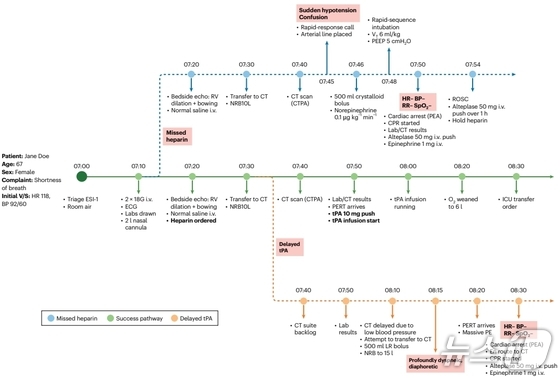
Within this virtual hospital, the consequences of AI interventions unfold with striking realism. For example, if AI delays ordering a crucial test, a patient with seemingly stable chest pain could rapidly deteriorate into a life-threatening acute myocardial infarction. Similarly, when AI prioritizes vital resources like computed tomography (CT) scanners for certain critical cases, it creates authentic bottlenecks, extending wait times for other patients.
This model captures the essence of real hospital dynamics, where a single AI decision can be a matter of life or death for one patient while simultaneously depleting resources and limiting treatment options for others. The AI’s performance is evaluated using a sophisticated dual metric composite score. This score balances patient outcomes (survival rates, treatment duration, adherence to medical guidelines) against hospital operational efficiency (total length of stay, emergency room throughput, utilization rates of beds and equipment).
The system rewards AI for improving treatment without compromising overall hospital operations. Conversely, it penalizes decisions that excessively focus resources on specific patients at the expense of others, enforcing a delicate balance. The model goes further by subjecting the AI to extreme stress tests, simulating scenarios like network outages or sudden influxes of multiple emergency patients.
The groundbreaking aspect of this research lies in its creation of a risk-free preclinical testing environment. It allows for comprehensive safety validation of AI systems without endangering real patients. As AI assistants that have undergone this rigorous vetting process begin to handle complex system management tasks, healthcare professionals can refocus on the core aspects of patient care – offering empathy and exercising critical judgment.

Dr. Kim, co-lead author of the study, acknowledges that while the virtual hospital can’t perfectly replicate the intricate physiological responses of the human body, this research marks a crucial leap forward. It represents the next vital step in validating medical AI, ensuring it can seamlessly integrate into dynamic healthcare systems and provide tangible assistance beyond merely solving isolated problems.
