A research team at Seoul St. Mary’s Hospital has developed an artificial intelligence (AI) model that accurately classifies pediatric emergency patients in the early stages of their hospital visit.
This innovative system is expected to streamline emergency room operations by quickly determining treatment priorities for young patients, who often struggle to articulate their symptoms clearly.
On Wednesday, Dr. Bae Woo-ri, Director of the Pediatric Emergency Medical Center at Catholic University of Korea Seoul St. Mary’s Hospital and Professor of Emergency Medicine, announced that their research team had developed and validated an AI-based model for early prediction of pediatric emergency cases. The findings were published in the prestigious international journal Scientific Reports.
The research team noted a steady increase in pediatric emergency room visits. While adults frequently seek emergency care for chronic conditions, children are more susceptible to infectious diseases, leading to higher emergency room (ER) visit rates among younger age groups.
According to the Health Insurance Review and Assessment Service, pediatric and adolescent emergency room visits reached 624,946 in 2024, marking a 7.3% increase from 2020. The most common diagnosis was other and unspecified fever.
However, pediatric patients often face challenges in accurately describing their symptoms compared to adults, making diagnosis more difficult. This issue is exacerbated in overcrowded emergency rooms, highlighting the need for a system that can quickly and accurately classify emergency cases.
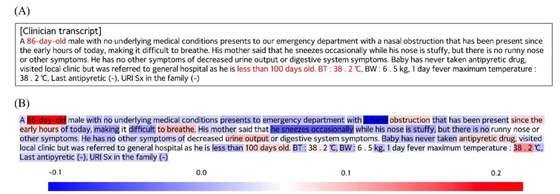
To address this, the research team employed natural language processing technology, enabling computers to analyze and interpret everyday language. This allowed them to examine symptoms and medical notes documented by healthcare professionals in electronic medical records.
Unlike traditional emergency patient classification methods that rely heavily on structured data such as vital signs and test results, the team recognized the value of clinical records made by medical staff before test results are available, as they often contain crucial information for assessing patient conditions.
The study analyzed electronic medical record data from 87,759 patients under 18 who visited a major Korean hospital’s pediatric emergency room between 2012 and 2021. Patients were categorized as either emergency or non-emergency cases.
Emergency patients were defined as those who underwent at least one of the following: blood tests, urinalysis, intravenous fluid therapy, inhalation therapy, emergency medication administration, or hospitalization. Non-emergency patients were those discharged with only oral medication prescriptions, without any tests or treatments.
The research team explained that to enhance accuracy, they classified patients based on actual treatment received, diverging from the current clinical practice of categorizing emergency patients into five levels (1-3 for emergency, 4-5 for non-emergency).
The team then developed a deep learning-based predictive model using the Korean Medical Natural Language Processing model (KM-BERT), which was trained on medical knowledge. They applied a masked language model (MLM) pre-training technique to the content of healthcare professionals’ medical records.
The resulting deep learning-based natural language processing model (KM-BERT with MLM) achieved an impressive 84% diagnostic accuracy (AUROC) and 88% diagnostic precision (AUPRC). This performance surpassed other machine learning-based models.
Moreover, when compared to the Korean Triage and Acuity Scale (KTAS), widely used in emergency rooms, the AI model demonstrated superior predictive accuracy.
Dr. Bae emphasized that in the emergency room, rapid assessment of a patient’s condition and determining treatment priorities is crucial. The AI’s analysis of clinical records allows for more accurate identification of emergency patients. He added that the future implementation of this technology in emergency rooms could significantly improve the efficient allocation of medical resources and enhance patient safety.

